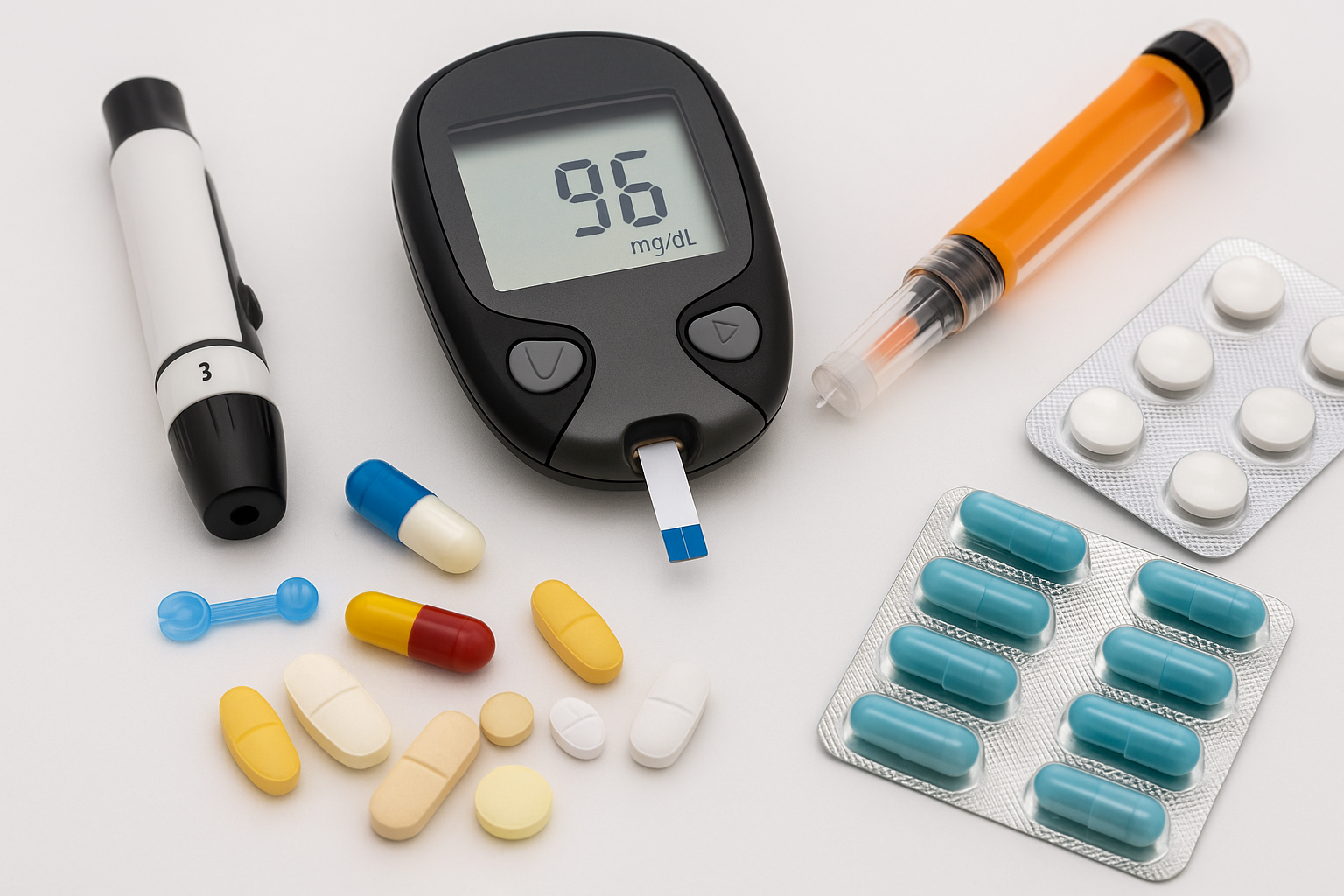
Understanding Diabetes and Medication Basics
Managing diabetes often involves lifestyle changes and medications. Medication choices depend on the type of diabetes (Type 1, Type 2, or other forms), blood glucose targets, other health conditions, cost, and personal preferences. This guide explains the major medication classes, how they work, common benefits and risks, and what to discuss with your healthcare team.
Oral Medications for Type 2 Diabetes
Many people with Type 2 diabetes start with oral medications. These drugs work in different ways to lower blood glucose and may be used alone or in combination.
Metformin
Metformin is often the first-line medication for Type 2 diabetes. It reduces glucose production in the liver and improves insulin sensitivity. It is affordable, effective for lowering A1C, and may support modest weight loss.
Common side effects: gastrointestinal upset (bloating, diarrhea) which often improves over time. Rarely, lactic acidosis can occur in people with advanced kidney disease.
Sulfonylureas and Meglitinides (Insulin Secretagogues)
Sulfonylureas (e.g., glipizide, glyburide) and meglitinides (e.g., repaglinide) stimulate the pancreas to release more insulin. They can be effective but have a higher risk of hypoglycemia (low blood sugar) and may contribute to weight gain.
Thiazolidinediones (TZDs)
TZDs (e.g., pioglitazone) improve insulin sensitivity. They can be effective for lowering A1C but may cause weight gain, fluid retention, and have links to heart failure risk in susceptible people.
Dipeptidyl Peptidase-4 (DPP-4) Inhibitors
DPP-4 inhibitors (e.g., sitagliptin) enhance the body’s incretin hormones to increase insulin release after meals. They are generally weight-neutral and have a low risk of hypoglycemia.
Sodium-Glucose Cotransporter-2 (SGLT2) Inhibitors
SGLT2 inhibitors (e.g., empagliflozin, canagliflozin) lower blood glucose by causing the kidneys to excrete excess sugar in urine. Benefits include weight loss and potential heart and kidney protection for some patients. Side effects can include urinary tract or genital infections and, rarely, dehydration or ketoacidosis.
Injectable Non-Insulin Options
GLP-1 Receptor Agonists
GLP-1 receptor agonists (e.g., liraglutide, semaglutide) mimic a gut hormone that increases insulin release, slows stomach emptying, and reduces appetite. These agents often promote weight loss and have cardiovascular benefits in certain patients. They are given by injection and can cause nausea that usually improves with time.
Insulin Therapy
Insulin is essential for Type 1 diabetes and commonly used in later stages of Type 2 diabetes when other medications are insufficient. Modern insulin options include basal (long-acting), bolus (rapid-acting), and premixed formulations. Many people use basal insulin to control fasting glucose and add rapid-acting insulin for meals.
Advances such as insulin pens, pumps, and continuous glucose monitoring (CGM) make insulin dosing safer and more convenient. The main risks are hypoglycemia and weight gain, but proper education and monitoring minimize these risks.
How Providers Choose a Medication
Treatment decisions are personalized. Providers consider:
- Type and duration of diabetes
- Current A1C and glucose patterns
- Other medical conditions (heart disease, kidney function)
- Risk of hypoglycemia
- Weight goals
- Cost, insurance coverage, and route of administration
Shared decision-making helps match the best medication plan to your life and priorities.
Side Effects, Interactions, and Safety
Every medication has potential side effects. Common themes include gastrointestinal symptoms (metformin, GLP-1s), hypoglycemia (insulin, sulfonylureas), and increased infection risk (SGLT2s). Kidney and liver function, heart disease, pregnancy, and other medications can affect which options are safe.
Always inform your provider about all medicines and supplements you take. Report severe side effects—such as severe abdominal pain, unexpected weakness, or signs of low blood sugar—promptly.
Monitoring and Adherence
Regular monitoring (home glucose checks and periodic A1C tests) helps track treatment effectiveness. Simple strategies to improve adherence include pill organizers, setting reminders, discussing side effects early, and addressing cost barriers with your care team.
Talking to Your Healthcare Team
Bring a list of questions to appointments: your goals, worries about side effects, concerns about injections, cost limits, and lifestyle factors. Ask about treatment benefits beyond glucose lowering—like effects on weight, heart, and kidneys.
Conclusion
There are many diabetes medication options, each with pros and cons. The right plan balances blood sugar control, safety, other health conditions, and your personal preferences. Work closely with your healthcare team to find and adjust the regimen that fits your life.
Note: This post is for informational purposes and not a substitute for medical advice. Always consult your healthcare provider before starting or changing medications.