What is Ulcerative Colitis?
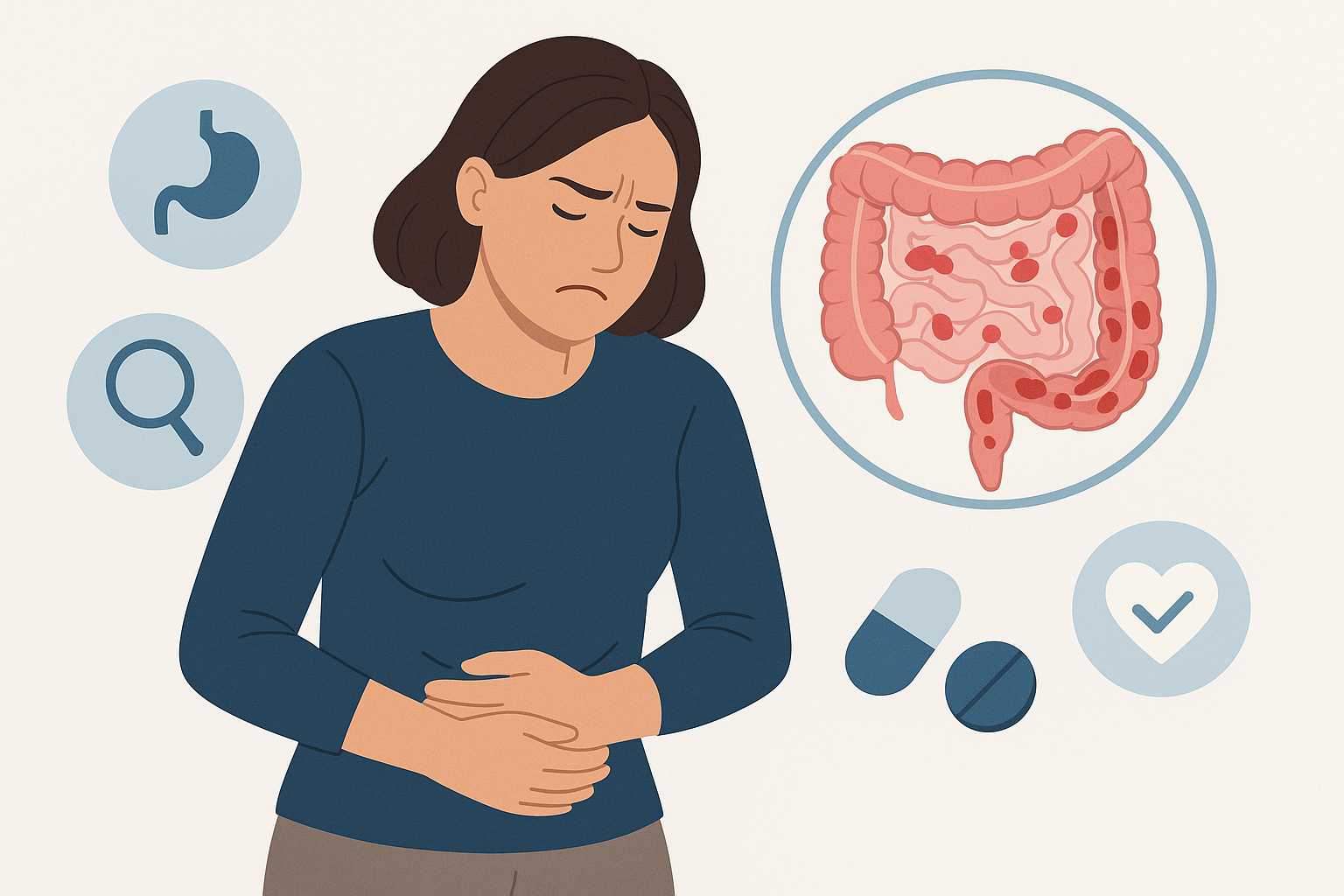
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) that causes inflammation and ulcers in the innermost lining of the large intestine (colon) and rectum. Unlike some other digestive conditions, UC affects the colon continuously and typically begins in the rectum, spreading upward to varying extents. Understanding UC helps people recognize symptoms early, seek appropriate care, and manage the condition effectively.
Definition and how it differs from Crohn’s
While ulcerative colitis and Crohn’s disease are both forms of IBD, they differ in where and how they affect the digestive tract. UC is limited to the colon and rectum and affects only the mucosal layer, whereas Crohn’s can affect any part of the gastrointestinal tract and penetrate deeper layers of the gut wall. These differences influence diagnosis and treatment decisions.
Who is affected?
Ulcerative colitis can develop at any age but often starts in late adolescence or early adulthood. It affects both men and women and occurs worldwide. Genetics, immune system factors, and environmental influences all play roles in who develops UC.
Common Symptoms
Digestive symptoms
The most common signs of ulcerative colitis relate to bowel function and include:
- Frequent, urgent bowel movements
- Bloody or pus-containing stools
- Abdominal pain and cramping, often on the lower left side
- Diarrhea that may be severe
- Weight loss and reduced appetite
Extraintestinal symptoms
UC can also cause symptoms outside the gut, such as joint pain, skin rashes, eye inflammation, and fatigue. These systemic symptoms reflect the inflammatory nature of the disease and may need coordinated care from specialists.
Causes and Risk Factors
Immune system and inflammation
Ulcerative colitis is believed to result from an abnormal immune response. Instead of protecting the body, the immune system mistakenly attacks cells in the colon, causing chronic inflammation and ulceration. What triggers this misdirected response is still being researched.
Genetics and environment
Family history increases risk—having a first-degree relative with UC raises the likelihood of developing it. Environmental factors such as urban living, diet, and certain medications may also influence risk, but no single cause has been identified.
Triggers
Although not causes, some factors can trigger flares or worsen symptoms: infections, nonsteroidal anti-inflammatory drugs (NSAIDs), stress, and certain foods. Individual triggers vary, so tracking symptoms can help identify personal patterns.
Diagnosis and Tests
Medical history and physical exam
Your clinician will take a detailed history of symptoms and medical background and perform a physical exam. Discussing family history and symptom patterns helps guide testing.
Endoscopy, imaging, labs
Key diagnostic tools include:
- Colonoscopy with biopsy: the gold standard for diagnosis and assessing disease extent
- Flexible sigmoidoscopy: used when colonoscopy isn’t immediately available or needed
- Blood tests: to check for anemia, inflammation, and markers of infection
- Stool tests: to rule out infections
- Imaging (CT or MRI): to evaluate complications or inflammation severity
Treatment Options
Medications
Treatment aims to reduce inflammation, induce remission, and maintain it. Medication classes include:
- Aminosalicylates (5-ASAs): useful for mild to moderate disease
- Corticosteroids: for short-term control of flares
- Immunomodulators and biologics: for moderate to severe UC or steroid-dependent disease
- JAK inhibitors: newer oral medications for certain patients
Surgery
Surgical removal of the colon (colectomy) can be curative for UC and may be recommended for severe disease, complications, or cancer risk. Many people do well after surgery, but it requires careful discussion and planning.
Lifestyle and diet strategies
While diet doesn’t cause UC, nutritional choices can influence symptoms. Working with a dietitian helps identify trigger foods, ensure adequate nutrition, and manage weight. Other helpful strategies include quitting smoking, regular exercise, and getting enough sleep.
Living with Ulcerative Colitis
Managing flares
Keep a symptom diary, stay in touch with your care team, and follow an action plan for flares. Early treatment of flare-ups often prevents complications and shortens recovery time.
Mental health and support
Living with a chronic condition can be stressful. Anxiety, depression, and social concerns are common. Seek mental health support, connect with IBD support groups, and lean on family and friends. Practical tips—like planning bathroom access when traveling—help preserve confidence and quality of life.
When to See a Doctor
Seek prompt medical attention for severe abdominal pain, high fever, heavy rectal bleeding, persistent vomiting, signs of dehydration, or sudden worsening of symptoms. Regular follow-ups are important to monitor disease activity and screen for complications, including colorectal cancer.
Conclusion
Ulcerative colitis is a manageable but chronic condition that affects each person differently. With early diagnosis, individualized treatment, lifestyle adjustments, and emotional support, many people with UC lead active, fulfilling lives. Partnering with your healthcare team and learning what works for your body are key steps toward long-term wellness.